Researchers monitor the brain with deep electrodes in patients suffering from epilepsy

Study the neuroscience of virtual reality through deep brain electrodes in patients.
This is a “unique” research project in the world, carried out by the Immersive Neurotechnologies Laboratory of the Universitat Politècnica de València (UPV), led by Professor Mariano Alcañiz; and the Functional Neurosurgery team at the La Fe hospital in Valencia, under the direction of neurosurgeon Antonio Gutiérrez.
The brain is still a “great mystery” for science, the last frontier of knowledge. For this reason, both institutions have joined forces to carry out research that will allow “answers to multiple unknowns about the functioning of the human brain.”
The group of academics has set out to decipher millions of neural connections and analyze them to understand the state of consciousness of the here and now or how the brain interprets reality.
These are unanswered questions that medicine and technology are focused on solving.
The joint project between the UPV and the La Fe hospital in Valencia has been presented at the VIII Congress of the Spanish Society of Functional and Stereotactic Neurosurgery of Valencia.
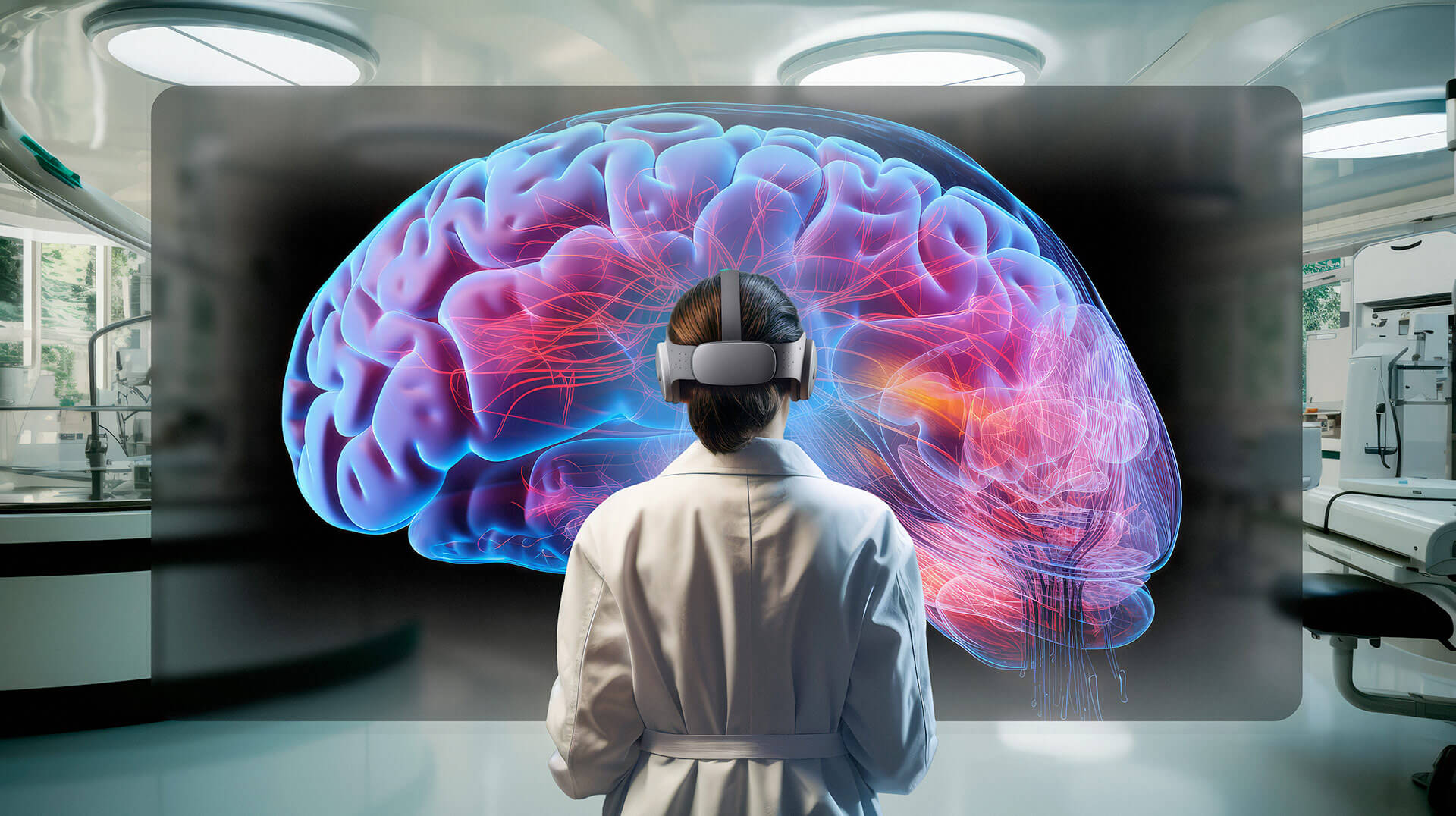
In this study, they implant deep brain electrodes in patients with epilepsy and, using a virtual reality helmet, subject them to virtual environments to measure the sense of presence in them.
The objective is to monitor how different brain areas communicate to respond to multiple unknowns about the functioning of the human brain in virtual environments.
It is, in the words of the UPV, “an open door to unexplored terrain, the brain, and that will help advance the use of the metaverse by better understanding how our brains behave when we are immersed in virtual reality.”
A unique field of research with philosophical overtones
In the conference ‘Studies of brain processing and state of consciousness. Monitoring using deep electrodes, Mariano Alcañiz stressed that it is a unique field of research with even philosophical connotations.
“Is human consciousness the same in virtual reality as in physical reality? We need to know what happens to the human brain when it is stimulated with an artificial reality,” the expert asked.
For Alcañiz we are facing “something similar to crossing the mirror of Alice in Wonderland”.
Brain monitoring with deep electrodes is being carried out in patients with epilepsy.

The process takes place uninterruptedly for several weeks, allowing for the collection of “large amounts of information” about brain impulses and reactions not so much during episodes of epileptic seizures as when normal, thinking and conscious brain functioning occurs.
“This collaboration is something that no one else in the world has. Finding a department that implants deep electrodes, that has a line of research and that also develops virtual reality is very difficult to achieve,” explained Dr. Antonio Gutiérrez, head Section of the Functional Neurosurgery Unit of the La Fe hospital.
What is functional neurosurgery?
It is the part of neurosurgery responsible for resolving abnormal brain function through surgical intervention.
It is applied in cases of epilepsy and surgery for movement disorders such as dystonia or Parkinson’s disease.
Virtual reality, an ally of neuroscience
Among the numerous treatments that exist to improve the quality of life of people who suffer from acquired neuronal damage, is neuro-rehabilitation. This relies on virtual reality to try to “trick” the brain, providing it with the illusion of movement from a first-person perspective.
In Spain, hospital centers such as the Arthros Clinic in Vigo are pioneers of this therapeutic application of virtual reality through the renowned FOREN Method, awarded in Amsterdam and Berlin with the “Halo Awards” for the best applications of virtual reality to neuroscience.
This method works with mirror neurons, responsible for imitation movements such as yawning, laughing or pain when seeing someone else’s hit.
The objective of this method is for the brain to “think, assimilate and completely believe” the order issued by itself through imitation thanks to observation with virtual reality.
Subsequently, therapists identify the patient’s motor and sensory response at the moment the movement should occur. In this way, the acquired damage is correctly evaluated and a unique and personalized solution can be worked on for each patient.
The healthcare sector relies on virtual and augmented reality (VR)
n addition to this research, at Etkho we have been talking at length about the possibilities of artificial intelligence and the most cutting-edge technological innovations applied to the healthcare environment.
One of these elements called to play a key role is augmented reality, which has already represented a huge change in terms of possibilities, safety and effectiveness in operating rooms.
This new health technology allows, among other things, it to be much easier for the surgeon or anesthetist to make life or death decisions during an operation, thanks for example to viewing organs in 3D, the patient’s vital signs, etc.
Virtual reality is also increasingly used in the rehabilitation of patients with neurological and physical injuries.
Without going any further, students and healthcare professionals can use VR devices to explore 3D anatomical models and practice virtual procedures before performing them on real patients.
Studies with great potential
Dr. Gutiérrez has also emphasized that the preliminary studies “are very encouraging. We are seeing how a patient, when shown a scene through virtual reality glasses, activates certain areas of the brain while remaining inactive when they are not shown.”
In addition, he highlighted the qualitative leap that this research with brain electrodes and virtual reality represents to decipher the functioning of the brain.
The reason?
The compilation of this data represents information for a lifetime of analysis:
“Sometimes I have the feeling like when man was on the Moon and brought back material and it is still being analyzed.”




